
What Is Psoriasis?
In Malaysia, up to 800,000 people are living with psoriasis. It affects 2-3% of the population and is more common than you think1. A widespread misconception is that psoriasis is just a skin disease because it often presents itself with red, itchy, and flaky skin.
In fact, psoriasis is not just an external disease but an internal one.
It’s a complex, chronic auto-immune disease that’s a result of several factors including genetics, the environment, and your immune system2.
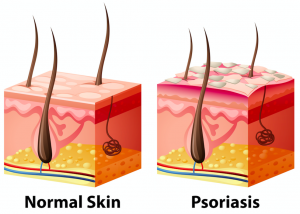
With psoriasis, the immune system mistakenly attacks healthy skin cells, causing the skin growth process to accelerate, leading to a build-up of dead skin cells on the surface of the skin3.
As a result, your skin becomes flaky, red, and inflamed. Since your immune system affects your whole body, psoriasis can manifest itself on different parts of your body simultaneously (although it typically affects the surface of the elbows, knees, or scalp)4.
Psoriasis is a chronic disease: once you have it, it doesn’t go away. Flare-ups may appear or subside depending on treatment and lifestyle choice. Most patients are diagnosed with psoriasis in early adulthood, with the average age of onset between 15 to 35 years old5 . The World Health Organization (WHO) estimates that about 75 percent of psoriasis cases are diagnosed before age 46.
For some patients, psoriasis is not just cosmetic — living day-to-day with this disease can affect their overall quality of life. It goes beyond physical appearances and often manifests itself through self-defeating thoughts.
66% of psoriasis patients face humiliation and discrimination. For 30%, their past or current relationships are affected. 55% took at least one day off from work in the last six months, and 48% say their professional lives are impacted7.
The biggest fear most people have when they first encounter this disease, is that psoriasis is contagious. Every psoriasis patient suffers differently.
It takes a team to help overcome these barriers to living normal lives. Understanding this complex disease is key; read on to separate fact from fiction.
Living with Psoriasis: Understanding 5 Basic Truths
1. Psoriasis is not infectious.
While scientists know that the immune system and genetic factors plays a role in psoriasis development, something external might cause flare-ups as well8. You can hug, kiss and have an intimate relationship with a person of psoriasis with no risk of directly contracting the disease yourself. It might run in families because some people can inherit the genes that make them prone to getting psoriasis but it doesn’t transmit by close contact. It’s okay to shake hands, breathe the same air, and share food with someone with psoriasis.

According to the National Psoriasis Foundation, research is still underway for scientists to understand the genes that trigger psoriasis in order to refine treatment solutions. ‘Scientists now believe that at least 10 percent of the general population inherits one or more of the genes that create a predisposition to psoriasis. [But] only two percent to three percent of people encounter the “right” mix of genetics and are exposed to triggers that lead to the development of psoriasis9‘.
2. Psoriasis has a major health impact on your whole body.
Psoriasis is a lifelong auto-immune disorder that puts you at risk of developing inflammation of multiple systems in your body, including joints.
A person with psoriasis has higher risk of getting hypertension, diabetes, heart disease, inflammatory bowel disease, and mood disorders such as depression10 .
The National Psoriasis Foundation emphasizes that if you have psoriasis, you need to work with your primary health care physician to reach a healthy weight, stop smoking, and control high blood pressure, cholesterol, and other metabolic problems11 .
In addition, if you have depression, anxiety, or experience social isolation as a byproduct of having psoriasis, then you need to reach out to the psoriasis community in Malaysia to hear information you need and learn about how to do things differently to manage your psoriasis. Feeling supported and understood by others suffering from the same condition will help you reduce stress12 .
An estimated 30 percent of people with psoriasis go on to develop psoriatic arthritis, with joint pain, stiffness, and swelling13. Please note that this is an inflammatory type of arthritis, not another form of psoriasis. The risk of not getting early recognition and treatment may be permanent joint damage14. Studies show, seeking treatment within six months is critical15 .
3. Not all psoriasis is the same.

There are several subcategories of psoriasis types. Knowing how to treat or manage psoriasis begins with figuring out the type of psoriasis you have and the severity with which symptoms present themselves.
Plaque psoriasis: The most common type; scaly plaques appear on your elbows and knees, but there are also variants that affect your scalp, lower back, or groin and armpit areas16. Plaque psoriasis causes raised, red patches covered with silvery, white scales. These patches may crack and bleed, they are often itchy and burn.
Guttate psoriasis: Children or younger adults can have guttate psoriasis after an episode of streptococcal sore throat — pink red spots (like rain-drops) appear on the trunk of your body. About 10% of psoriasis patients may develop this17.
Inverse psoriasis: Inverse psoriasis is a variant of psoriasis that appears as scaly plaques on extensors (elbows, knees) and flexures (where the skin opposes each other such as the groin area and armpits). You could have inverse psoriasis and another type of psoriasis elsewhere on your body simultaneously18.
Pustular psoriasis is characterized by white pustules, pus-filled blisters surrounded by red skin. The pus consists of white blood cells, and normally occurs on the hands or feet19.
Erythrodermic psoriasis affects almost all the skin on the body, causing fiery skin that appears burned. You may have severe itching, and your skin could come off in sheets. Very rare, it occurs in 3 percent of patients who have unstable plaque psoriasis20.
These subtypes of psoriasis are not exclusive, which means that a person with plaque psoriasis may develop pustular psoriasis or progress into erythrodermic psoriasis. Guttate psoriasis can be potentially cured but may progress into plaque psoriasis too.
Psoriasis shows up differently on different areas of your body — on the eyelids, ears, mouth and lips, skin folds, hands and feet, and nails. The skin at each of these sites is different and requires different treatments21.
Nail psoriasis affects up to half of those with psoriasis. Common symptoms include cracking, blisters, and swelling on your nails. You could also have nail pitting, deformations, thickening, discoloration, and separation of nail from the nail bed22.
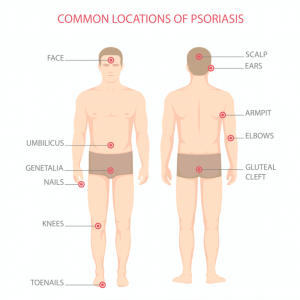
Scalp psoriasis can affect half of psoriasis patients. It ranges in severity, from mild, fine, scaling to crusted plaques that cover the entire scalp. Be aware that scalp psoriasis can also appear on your forehead, the back of your neck and around your ears23.
4. Lifestyle choices and environmental factors trigger psoriasis24.
Psoriasis triggers differ by individual on a case-by-case basis. You need to learn to recognize triggers particular to your case of psoriasis and track them in order to make positive lifestyle choices.
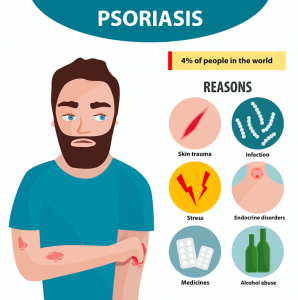
Triggers include, but are not limited to: smoking, alcohol, stress, injury to skin (vaccinations, cuts, scrapes, sunburns, scratches, or even a tattoo), certain medications, infections, allergies, diet, and weather25.
Make smart lifestyle choices while you’re on psoriasis treatments. Give up smoking, and alcohol. Schedule daily relaxation periods and try to reduce your own stress levels. Exercise and be wary of medications and foods that may cause flare-ups.
5. There is no cure for psoriasis.
While there isn’t a “cure” yet, psoriasis is very treatable. There are many ways to treat psoriasis, not just with topical creams. Treatment depends on the type of psoriasis you have, the severity, and the area affected.
When you see your dermatologist, you might be given topical creams, phototherapy, oral tablets or injections. It’s important to set realistic treatment goals, and continuously monitor your progress. Individuals respond differently to treatments and may have to cycle through treatment options over time to see results.
Topical treatments such as moisturizers, creams, and ointments can reduce itching, inflammation, and redness of lesions. In the short term, drugs may be prescribed to reduce flare-ups such as topical corticosteroids or topical retinoids26.
Light therapy (using natural or artificial ultraviolet light) is the simplest and easiest form of treatment, used alone or in combination with other medications.
Brief, daily exposures to small amounts of sunlight may improve psoriasis, but intense sun exposure can worsen symptoms and cause skin damage. Controlled exposures through laser treatments allow for UVB to work on targeted areas. Consult your doctor about the safest way to use light therapy for psoriasis treatment27.
Systemic medications are prescription drugs that work throughout the body. They are usually prescribed for moderate to severe psoriasis and psoriatic arthritis. Systemic treatments include acitretin, methotrexate, and cyclosporine28.
Biologics are different from the traditional systemic drugs as it targets specific parts of the immune system. Biologics are prescribed for individuals with moderate to severe cases of plaque psoriasis and psoriatic arthritis29.
Staying Informed Means Staying in Control of Your Psoriasis

Chronic diseases such as psoriasis require you to be a proactive agent in your own healthcare and a strong advocate for your own well-being. Now that you’re better informed, you have a starting point from which to manage your psoriasis triggers, learn about treatment plans, seek support, and make lifestyle choices.
Track your progress keenly so that you can have an open conversation with your doctor to get the best treatment for your skin. Before treatment, list down your symptoms, medications or dietary supplements you’re taking, and treatments you’re interested in.
During treatment, be patient, stay compliant to doctor’s orders, and give it about 8-12 weeks before expecting results. Always stay in touch with your doctor and do not give up.
Visit our Facebook page to find out more information about psoriasis.
Read stories like this and more about psoriasis on our Stay Informed page.
#Ask4Clear skin to lead a normal life. Find a dermatologist near you today.
If you enjoyed this article, read Biologic Treatment for Psoriasis: 4 Things You Need to Know
References
1 https://psoriasismalaysia.wordpress.com/about/
2 https://www.psoriasis.org/about-psoriasis
3 Krueger G. Arch Dermatol 2001; 137:280-84.
4, 5 https://www.psoriasis.org/about-psoriasis
6 https://www.healthline.com/health/psoriasis#statistics
7 http://www.skintolivein.in/psoriasis/what-is-psoriasis/
8, 10 https://www.psoriasis.org/about-psoriasis
9 https://www.psoriasis.org/research/genes-and-psoriatic-disease
11 https://www.psoriasis.org/advance/the-whole-body-effect-of-psoriatic-disease
12 https://psoriasismalaysia.wordpress.com/about/
13 https://www.psoriasis.org/psoriatic-arthritis
14, 15 https://www.psoriasis.org/about-psoriatic-arthritis
16, 17, 18, 19, 20, 21 https://www.psoriasis.org/about-psoriasis
22 https://www.psoriasis.org/about-psoriasis/specific-locations/hands-feet-nails
23 https://www.psoriasis.org/about-psoriasis/specific-locations/scalp
24, 25 https://www.psoriasis.org/about-psoriasis/causes
26 https://www.psoriasis.org/about-psoriasis/treatments/topicals
27 https://www.psoriasis.org/about-psoriasis/treatments/phototherapy
28 https://www.psoriasis.org/about-psoriasis/treatments/systemics
29 https://www.psoriasis.org/about-psoriasis/treatments/biologics






